Home ►
help ►
Fee schedule lookup tool - help guide
Last Modified: 5/15/2024
Location: FL, PR, USVI
Business: Part A, Part B
The
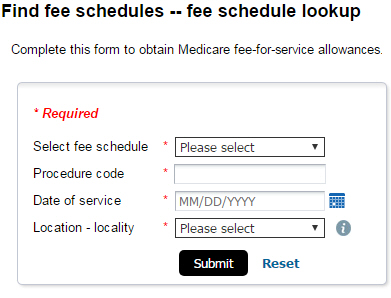
fee schedule lookup tool was designed to provide users a more simplified approach to obtaining appropriate fee and policy information for most Medicare-covered procedure codes.
1. Select Fee Schedule -- select the appropriate fee schedule from the drop-down menu.
• Part A Options include:
• Ambulance
• ASP (Average Sales Price) Drugs
• Clinical Lab
• DMEPOS (Durable medical equipment, prosthetics, orthotics, and supplies)
• Mammography
• Outpatient Rehabilitation
• Part B Options include:
• Ambulance
• Anesthesia
• ASC (Ambulatory Surgical Center)
• ASC Drugs
• ASP (Average Sales Price) Drugs
• Clinical Lab
• DMEPOS (Durable medical equipment, prosthetics, orthotics, and supplies)
• Medicare Physician and Nonphysician Practitioner Fee Scheduled (MPFS)
Note: You must change your line of business to view the alternative listing. To locate your current line of business, look under the First Coast logo, in the left navigation column. To change, simply click on the Part A or Part B link shown, and you will be prompted to select your settings.
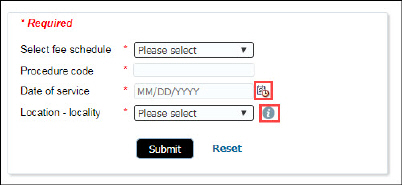
2. Date of Service -- enter the date of service in the format of MM/DD/YYYY or click the calendar icon to select your date.
• Options for Florida include:
• Florida-03
• Florida-04
• Florida-99
• Options for Puerto Rico include:
• Puerto Rico-20
• Options for U.S. Virgin Islands include:
• U.S. Virgin Islands-50
4. County/Municipality (required for ASC and ASC Drugs) – select the county/municipality for the location of service
5. Procedure Code – enter the procedure code for the service provided (for example: 66984) and click the “Submit” button.
Upon completing the short form and clicking the “Submit” button, the appropriate fee schedule data will be displayed based upon the information inputted.
Note: If you change information on the fee schedule lookup tool, such as “Date of Service”, you must click the “Submit” button again to update the results.
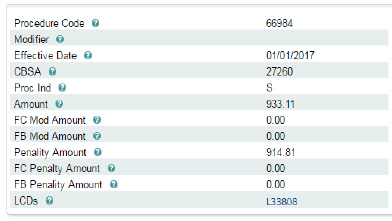
Example of the results for ASC – procedure code 66984:
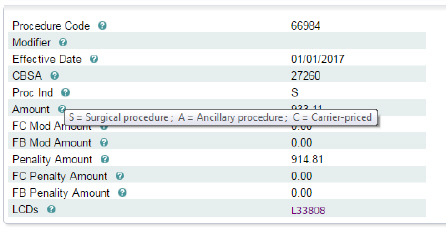
Results -- The results will vary upon the information inputted. The results for ASC-- 66984 provide the following information:
• Procedure Code (The Current Procedural Terminology (CPT®) code assigned by the American Medical Association (AMA) or the Healthcare Common Procedure Coding System (HCPCS) code assigned by the Centers for Medicare & Medicaid Services (CMS) that describes the service)
• Modifier (For ASC facility services, a blank in this field denotes the ASC facility service; TC = technical component only)
• Effective Date (Date the fee for the date of service requested became effective)
• CBSA (Core-based statistical areas used to determine geographic payment differences for ASC facility services)
• Proc Ind (procedure type indicator -- S = surgical procedure, A = ancillary service, C = carrier-priced)
• Amount (Allowed amount for the ASC facility service requested)
• FC Mod Amount (FC modifier = Item provided without cost to provider, supplier or practitioner, or full credit received for replaced device (examples, but not limited to, covered under warranty, replaced due to defect, free samples))
• FB Mod Amount (FB modifier = Partial credit received for replaced device)
• Penalty Amount (ASCFS Quality penalty payment amount for surgical and ancillary services)
• FC Penalty Amount (FC Modifier Penalty Price)
• FB Penalty Amount (FB Modifier Penalty Price)
• LCDs (Current and proposed local coverage determination(s) applicable to the procedure code requested. For previous versions of an LCD, refer to the CMS Medical Coverage Database. If blank, no current LCD exists for the procedure.)
LCDs -- In the example above, an LCD is associated with the procedure code entered. When present, the “LCD number” is a clickable link which directs users to information related to the LCD. Once clicked, a new window will appear with LCD information such as contractor information, coding information, and much more. Note: You may need to turn off your pop-up blocker to view this page.
Tooltips -- The majority of the column headers contain a “?” next to the title. When the cursor is placed over any of these items, helpful tooltips will appear, providing a description for each category. Below is an example of the Proc Ind tooltip:
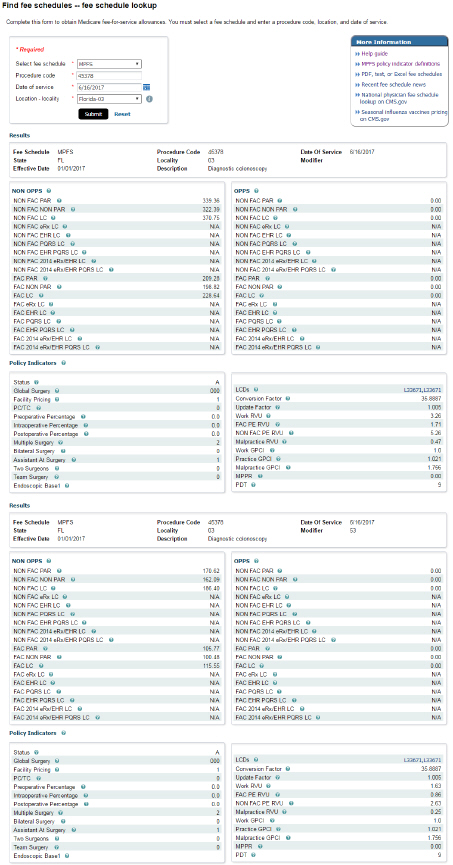
Example of the results for MPFS -- procedure code 45378:
Results -- As mentioned, the results displayed will vary depending on the fee schedule and procedure code entered. The results for MPFS – 45378 provide the following information:
• Fee Schedule (Fee schedule selected)
• Procedure Code (The Current Procedural Terminology (CPT) code assigned by the American Medical Association (AMA) or the Healthcare Common Procedure Coding System (HCPCS) code assigned by the Centers for Medicare & Medicaid Services (CMS) that describes the service)
• Date of Service (Date of service selected)
• State/Territory (State or territory selected)
• Locality (Locality selected: 03 = Fort Lauderdale, FL, 04 = Miami, FL, 99 (01/02) = Florida, rest of state; 20 = Puerto Rico; 50 = U.S. Virgin Islands
• Modifier (For diagnostic procedures, a blank in this field denotes the global service and the following modifiers identify the components: 26 = Professional component, TC = Technical component. For services other than those with a professional and/or technical component, this field is blank with one exception: modifier 53 indicates that separate relative value units (RVUs) and a fee schedule amount have been established for procedures terminated before completion.)
• Effective Date (Date the fee schedule for the date of service selected became effective)
• Description (Abbreviated description of the procedure code requested. For a complete description of the service, refer to the Current Procedural Terminology (CPT) code book published by the American Medical Association (AMA) or the Healthcare Common Procedure Coding System (HCPCS) code assigned by the Centers for Medicare & Medicaid Services (CMS).)
• NON-OPPS (Payment for the technical component not capped at the outpatient prospective payment system amount.)
• NON FAC PAR (Allowance for participating physician or nonphysician practitioner when service is not performed in a facility setting.)
• NON FAC NON PAR (Allowance for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting)
• NON FAC LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting)
• NON FAC eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with eRx negative adjustment)
• NON FAC EHR LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR negative adjustment)
• NON FAC PQRS LC(Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with PQRS negative adjustment)
• NON FAC EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR and PQRS negative adjustment)
• NON FAC 2014 eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR and 2014 eRx negative adjustment)
• NON FAC 2014 EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR, 2014 eRx, and PQRS negative adjustment)
• FAC PAR (Allowance for participating physician or nonphysician practitioner when service is performed in a facility setting)
• FAC NON PAR (Allowance for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting)
• FAC LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting)
• FAC eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with eRx negative adjustment)
• FAC EHR LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR negative adjustment)
• FAC PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with PQRS negative adjustment)
• FAC EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR and PQRS negative adjustment)
• FAC 2014 eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR and 2014 eRx negative adjustment)
• FAC 2014 EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR, 2014 eRx, and PQRS negative adjustment)
• OPPS (Payment for the technical component is capped at the outpatient prospective payment system amount. When present, use these amounts if lower than NON-OPPS amounts.)
• NON FAC PAR (Allowance for participating physician or nonphysician practitioner when service is not performed in a facility setting)
• NON FAC NON PAR (Allowance for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting)
• NON FAC LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting)
• NON FAC eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with eRx negative adjustment)
• NON FAC EHR LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR negative adjustment)
• NON FAC PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with PQRS negative adjustment)
• NON FAC EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR and PQRS negative adjustment)
• NON FAC 2014 eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR and 2014 eRx negative adjustment)
• NON FAC 2014 EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is not performed in a facility setting with EHR, 2014 eRx, and PQRS negative adjustment)
• FAC PAR (Allowance for participating physician or nonphysician practitioner when service is performed in a facility setting)
• FAC NON PAR (Allowance for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting)
• FAC LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting)
• FAC eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with eRx negative adjustment)
• FAC EHR LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR negative adjustment)
• FAC PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with PQRS negative adjustment)
• FAC EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR and PQRS negative adjustment)
• FAC 2014 eRx LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR and 2014 eRx negative adjustment)
• FAC 2014 EHR PQRS LC (Limiting charge for nonparticipating physician or nonphysician practitioner when service is performed in a facility setting with EHR, 2014 eRx, and PQRS negative adjustment)
Policy Indicators (Medicare physician fee schedule payment policy indicators --
click here for more information)
• Status (Provides the fee schedule status of each procedure code)
• Global Surgery (Provides the postoperative time frames that apply to payment for each surgical procedure or another indicator that describes the applicability of the global concept to the service)
• Facility Pricing (Facility fees are calculated at a national level with a reduced practice expense because of reduced physician overhead associated with services provided in a facility)
• PC/TC (Professional component/technical component indicator)
• Preoperative Percentage (Provides the percentage for the preoperative portion of the global package)
• Intraoperative Percentage (Provides the percentage for the intraoperative portion of the global package including postoperative work in the hospital)
• Postoperative Percentage (Provides the percentage for the postoperative portion of the global package that is provided in the office after discharge from the hospital)
• Multiple Surgery (Indicates which payment adjustment rule for multiple procedures applies to the service)
• Bilateral Surgery (Provides an indicator for services subject to a payment adjustment when performed bilaterally)
• Assistant at Surgery (Provides an indicator for services where an assistant at surgery may or may not be paid)
• Two Surgeons (Provides an indicator for services for which two surgeons, each in a different specialty, may be paid)
• Team Surgery (Provides an indicator for services for which team surgeons may be paid)
• Endoscopic Base1 (Identifies an endoscopic base code for each code with a multiple surgery indicator of 3. If an endoscopic procedure is reported with only its base procedure, the base procedure may not be paid separately. Payment for the base procedure is included in the payment for the other endoscopy.)
• LCDs (Current and proposed local coverage determination(s) applicable to the procedure code requested. For previous versions of an LCD, refer to the CMS Medical Coverage Database. If blank, no current LCD exists for the procedure.)
• Conversion Factor (Provides the multiplier which transforms relative values into payment amounts)
• Update Factor (The update factor is included in the conversion factor)
• Work RVU (Provides the unit value for the physician work Relative Value Unit)
• FAC PE RVU (Provides the unit value for the practice expense RVU in a facility setting)
• NON FAC PE RVU (Provides the unit value for the practice expense RVU in a non-facility setting)
• Malpractice RVU (Provides the unit value for the malpractice expense RVU)
• Work GPCI (Provides a work geographic adjustment factor used in computing the fee schedule amount)
• Practice GPCI (Provides a practice expense geographic adjustment factor used in computing the fee schedule amount)
• Malpractice GPCI (Provides a malpractice expense geographic adjustment factor used in computing the fee schedule amount)
• MPPR (Provides the reduced therapy fee schedule amount for multiple therapy procedures (eff. 1/1/2011))
• PDT (Provides an indicator for purchased diagnostic test codes (eff. 1/1/2014))
Modifiers -- In the example above, there are multiple modifiers displayed. Information related to each modifier is listed in a separate section.
LCDs -- Also in this example there are two LCDs associated with the procedure code (MPFS -- 45378), each a clickable link directing the user to LCD information.
More information – In the right column, users can find “More information”, which easily provides the opportunity to obtain more information such as fee schedule downloads, news, and relevant information on the CMS website.
• ASP – Average sales price
• CBSA – Core-based statistical areas
• DME – Durable medical equipment
• ESRD – End stage renal disease
• FAC LC - Limiting charge in a facility setting
• FAC PAR – Facility setting, participating physician or nonphysician practitioner
• FB Mod – Partial credit modifier
• FC Mod - Full credit modifier
• GAF – Geographic adjustment factor
• GPCI – Geographic practice cost index
• LCD – Local coverage determination
• NON FAC LC – Limiting charge in a non-facility setting
• NON FAC NON PAR – Non-facility setting, nonparticipating physician or nonphysician practitioner
• NON FAC PAR – Non-facility setting, participating physician or nonphysician practitioner
• NON FAC PE GPCI – Geographic practice cost index
• NON-OPPS – Not capped at the outpatient prospective payment system amount
• OPPS – Capped at the outpatient prospective payment system amount
• PC/TC – Professional component/Technical component indicator
• Proc Ind – Procedure indicator
• RVU – Relative value unit
• Supv DX – Supervision required for diagnostic codes
First Coast Service Options (First Coast) strives to ensure that the information available on our provider website is accurate, detailed, and current. Therefore, this is a dynamic site and its content changes daily. It is best to access the site to ensure you have the most current information rather than printing articles or forms that may become obsolete without notice.