Home ►
Help ►
Coming in September: Get ready to explore the new landscape of medicare.fcso.com
Last Modified: 8/29/2025
Location: FL, PR, USVI
Business: Part A, Part B
First Coast’s No. 1 provider resource – medicare.fcso.com – will soon be replaced by a new, modernized website experience. Featuring a modern look and feel with improved search and navigation abilities, our new provider website will continue to give you the same tools and valuable information that you need and enjoy, with the highest-quality content and resources being easier to locate for everyday use.
At First Coast, we are proud to reach the pinnacle in provider support for our users. As we ascend to the launch date, we will prepare you to navigate a new and exciting web-based landscape. You will love what we have waiting for you!
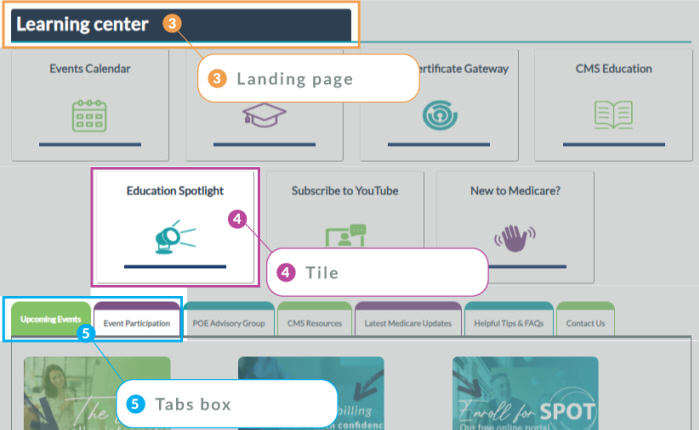
Our navigation transitioned from left navigation to the top of the screen, featuring five main areas of focus: Claims & EDI, Enrollment, Learning Center, Policy & Review Programs, and Tools & Forms.
• Claims & EDI (Electronic Data Interchange): This is where you’ll find resources relating to Medicare claims and appeals, including billing and coding information, the Fee Schedule Lookup Tool, Modifier Lookup Tool, Appeals Status Tool, and the Reopening Gateway. Electronic services, including our popular SPOT portal, can also be found here.
• Enrollment: This section features provider enrollment-related resources and articles, online enrollment options via PECOS and the Enrollment Gateway, where to find the status of an application, and the Application Assistance Tool.
• Learning Center: Our wide-ranging Events Calendar can be found in this area, as well as On-Demand Learning resources, the MyCEUCertificate Gateway, and an area dedicated for those of you who are new to the Medicare program.
• Policy & Review Programs: This is the place to find the LCD Interactive Index, prior authorization information, CERT program resources, and other information related to medical policy and review.
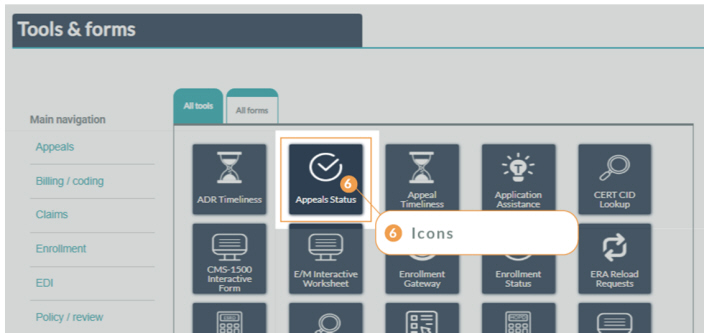
• Tools & Forms: Find all your favorite self-service tools in this spot, as well as a consolidated repository for forms, such as claims forms, enrollment forms, EDI forms, and more.
Consistently accessible throughout the new website experience is the utility bar located in the top right corner of the site. Here, you’ll find a quick access button for logging into our SPOT portal, FAQs and global site search options, and an area dedicated to provider/facility specialties and services.
For users who prefer a visibly expanded set of choices when browsing, the topics selection provides a complete site map of topics and areas included on our website for quick access.
For those looking to access Spanish content, the Español link will instantly translate the viewed page to Spanish for easy toggling between English and Spanish sites.
Find phone numbers and other contact options faster by clicking the phone icon, on the utility bar, at the top right of the homepage. There, you’ll find Provider Contact Center phone numbers, mailing addresses, and online inquiry links all in one place. Plus, view live system status updates, including SPOT and the Interactive Voice Response (IVR).
The envelope icon on the utility bar leads you to subscribe to our eNews emails (delivered to your inbox every Tuesday and Friday), so you can be the first to learn of new Medicare updates and other essential information.
As always, clicking the First Coast logo at the top left will take you back to the homepage.
Links to the latest Medicare news can now be easily accessed at the center of the homepage, as well as within customized tabs (5) throughout new topic-based landing pages (3). These areas are where you can easily see the latest articles and announcements at a glance.
The new web-platform accommodates more screens and devices than ever before. The new website adapts to computer screens of all sizes, as well as phones and tablets for a better viewing and navigation experience in all settings.
We’ve created a simple, attractive, tile and icon-based design throughout the website for a clean, easy representation of our content. Clickable tiles on our landing pages and icons on our tool pages and top navigation direct you to the content and features you use the most.
The new website offers all of the content, resources and tools you were accustomed to using on the archived platform. Our goal with the new design is to streamline navigation and promote accessibility of the information that matters most to you.
View our videos for additional highlights of our upcoming redesign:
We’re excited for you to begin using the new provider website, coming this September. More news, including your opportunity to attend first-look demonstrations, is coming soon. Visit our
Event Calendar to register for our webinars in August “Unveiling the New First Coast Provider Website” for a sneak peak of the new site.
First Coast Service Options (First Coast) strives to ensure that the information available on our provider website is accurate, detailed, and current. Therefore, this is a dynamic site and its content changes daily. It is best to access the site to ensure you have the most current information rather than printing articles or forms that may become obsolete without notice.