LICENSE FOR USE OF "PHYSICIAN'S CURRENT PROCEDURAL TERMINOLOGY" (CPT), FOURTH
EDITION End User/Point and Click Agreement: CPT codes, descriptions and other
data only are copyright 2022 American Medical Association (AMA).
All Rights Reserved (or such other date of publication of CPT). CPT is a
trademark of the AMA.
You, your employees, and agents are authorized to use CPT only as contained
in the following authorized materials:
Local Coverage Determinations (LCDs),
Local Medical Review Policies (LMRPs),
Bulletins/Newsletters,
Program Memoranda and Billing Instructions,
Coverage and Coding Policies,
Program Integrity Bulletins and Information,
Educational/Training Materials,
Special mailings,
Fee Schedules;
internally within your organization within the United States for the sole use
by yourself, employees and agents. Use is limited to use in Medicare,
Medicaid, or other programs administered by the Centers for Medicare and
Medicaid Services (CMS), formerly known as Health Care Financing
Administration (HCFA). You agree to take all necessary steps to insure that
your employees and agents abide by the terms of this agreement. Any use not
authorized herein is prohibited, including by way of illustration and not by
way of limitation, making copies of CPT for resale and/or license,
transferring copies of CPT to any party not bound by this agreement, creating
any modified or derivative work of CPT, or making any commercial use of CPT.
License to use CPT for any use not authorized here in must be obtained through
the AMA, CPT Intellectual Property Services, 515 N. State Street, Chicago, IL
60610. Applications are available at the AMA website. Applicable FARS/DFARS restrictions apply to government use.
AMA Disclaimer of Warranties and Liabilities CPT is provided "as is" without warranty of any kind, either expressed or
implied, including but not limited to, the implied warranties of
merchantability and fitness for a particular purpose. No fee schedules, basic
unit, relative values or related listings are included in CPT. The AMA does
not directly or indirectly practice medicine or dispense medical services. The
responsibility for the content of this file/product is with CMS and no
endorsement by the AMA is intended or implied. The AMA disclaims
responsibility for any consequences or liability attributable to or related to
any use, non-use, or interpretation of information contained or not contained
in this file/product. This agreement will terminate upon notice if you violate
its terms. The AMA is a third party beneficiary to this agreement.
CMS Disclaimer: The scope of this license is determined by the AMA, the copyright holder. Any
questions pertaining to the license or use of the CPT must be addressed to the
AMA. End Users do not act for or on behalf of the CMS. CMS DISCLAIMS
RESPONSIBILITY FOR ANY LIABILITY ATTRIBUTABLE TO END USER USE OF THE CPT. CMS
WILL NOT BE LIABLE FOR ANY CLAIMS ATTRIBUTABLE TO ANY ERRORS, OMISSIONS, OR
OTHER INACCURACIES IN THE INFORMATION OR MATERIAL CONTAINED ON THIS PAGE. In
no event shall CMS be liable for direct, indirect, special, incidental, or
consequential damages arising out of the use of such information or material.
AMA - U.S. Government Rights
This product includes CPT which is commercial technical data and/or computer
data bases and/or commercial computer software and/or commercial computer
software documentation, as applicable which were developed exclusively at
private expense by the American Medical Association, 515 North State Street,
Chicago, Illinois, 60610. U.S. Government rights to use, modify, reproduce,
release, perform, display, or disclose these technical data and/or computer
data bases and/or computer software and/or computer software documentation are
subject to the limited rights restrictions of DFARS 252.227-7015(b)(2)(June
1995) and/or subject to the restrictions of DFARS 227.7202-1(a)(June 1995) and
DFARS 227.7202-3(a )June 1995), as applicable for U.S. Department of Defense
procurements and the limited rights restrictions of FAR 52.227-14 (June 1987)
and/or subject to the restricted rights provisions of FAR 52.227-14 (June
1987) and FAR 52.227-19 (June 1987), as applicable, and any applicable agency
FAR Supplements, for non-Department Federal procurements.
ADA CURRENT DENTAL TERMINOLOGY, (CDT)
End User/Point and Click Agreement: These materials contain Current Dental
Terminology (CDTTM), Copyright © 2016 American Dental Association (ADA).
All rights reserved. CDT is a trademark of the ADA.
THE LICENSE GRANTED HEREIN IS EXPRESSLY CONDITIONED UPON YOUR ACCEPTANCE OF
ALL TERMS AND CONDITIONS CONTAINED IN THIS AGREEMENT. BY CLICKING ON THE
BUTTON LABELED "ACCEPT", YOU HEREBY ACKNOWLEDGE THAT YOU HAVE READ, UNDERSTOOD
AND AGREED TO ALL TERMS AND CONDITIONS SET FORTH IN THIS AGREEMENT.
IF YOU DO NOT AGREE WITH ALL TERMS AND CONDITIONS SET FORTH HEREIN, CLICK ON
THE BUTTON LABELED "DECLINE" AND EXIT FROM THIS COMPUTER SCREEN.
IF YOU ARE ACTING ON BEHALF OF AN ORGANIZATION, YOU REPRESENT THAT YOU ARE
AUTHORIZED TO ACT ON BEHALF OF SUCH ORGANIZATION AND THAT YOUR ACCEPTANCE OF
THE TERMS OF THIS AGREEMENT CREATES A LEGALLY ENFORCEABLE OBLIGATION OF THE
ORGANIZATION. AS USED HEREIN, "YOU" AND "YOUR" REFER TO YOU AND ANY
ORGANIZATION ON BEHALF OF WHICH YOU ARE ACTING.
Subject to the terms and conditions contained in this Agreement, you, your
employees and agents are authorized to use CDT only as contained in the
following authorized materials and solely for internal use by yourself,
employees and agents within your organization within the United States and its
territories. Use of CDT is limited to use in programs administered by Centers
for Medicare & Medicaid Services (CMS). You agree to take all necessary
steps to ensure that your employees and agents abide by the terms of this
agreement. You acknowledge that the ADA holds all copyright, trademark and
other rights in CDT. You shall not remove, alter, or obscure any ADA copyright
notices or other proprietary rights notices included in the materials.
Any use not authorized herein is prohibited, including by way of illustration
and not by way of limitation, making copies of CDT for resale and/or license,
transferring copies of CDT to any party not bound by this agreement, creating
any modified or derivative work of CDT, or making any commercial use of CDT.
License to use CDT for any use not authorized herein must be obtained through
the American Dental Association, 211 East Chicago Avenue, Chicago, IL 60611.
Applications are available at the ADA website.
Applicable Federal Acquisition Regulation Clauses (FARS)\Department of
restrictions apply to Government Use.
ADA DISCLAIMER OF WARRANTIES AND LIABILITIES: CDT is provided "as is" without
warranty of any kind, either expressed or implied, including but not limited
to, the implied warranties of merchantability and fitness for a particular
purpose. No fee schedules, basic unit, relative values or related listings are
included in CDT. The ADA does not directly or indirectly practice medicine or
dispense dental services. The sole responsibility for the software, including
any CDT and other content contained therein, is with (insert name of
applicable entity) or the CMS; and no endorsement by the ADA is intended or
implied. The ADA expressly disclaims responsibility for any consequences or
liability attributable to or related to any use, non-use, or interpretation of
information contained or not contained in this file/product. This Agreement
will terminate upon notice to you if you violate the terms of this Agreement.
The ADA is a third party beneficiary to this Agreement.
CMS DISCLAIMER: The scope of this license is determined by the ADA, the
copyright holder. Any questions pertaining to the license or use of the CDT
should be addressed to the ADA. End Users do not act for or on behalf of the
CMS. CMS DISCLAIMS RESPONSIBILITY FOR ANY LIABILITY ATTRIBUTABLE TO END USER
USE OF THE CDT. CMS WILL NOT BE LIABLE FOR ANY CLAIMS ATTRIBUTABLE TO ANY
ERRORS, OMISSIONS, OR OTHER INACCURACIES IN THE INFORMATION OR MATERIAL
COVERED BY THIS LICENSE. In no event shall CMS be liable for direct, indirect,
special, incidental, or consequential damages arising out of the use of such
information or material.
End Disclaimer



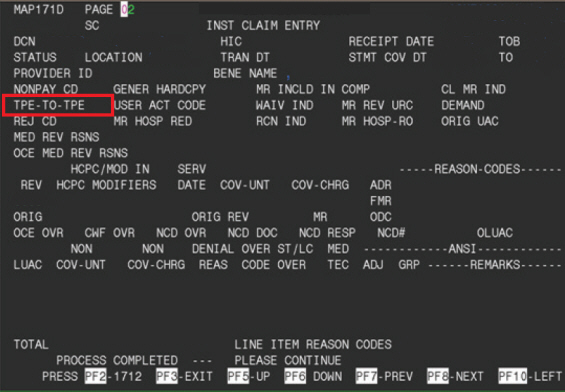
 ; Medicare Part A Direct Data Entry (DDE) Training Manual
; Medicare Part A Direct Data Entry (DDE) Training Manual 