Home ►
Medical review ►
Targeted probe and educate (TPE) round results - Evaluation and Management services - Outpatient Established Office Visits
Last Modified: 7/25/2025
Location: FL, PR, USVI
Business: Part A, Part B
Evaluation and Management services – Outpatient Established Office Visits
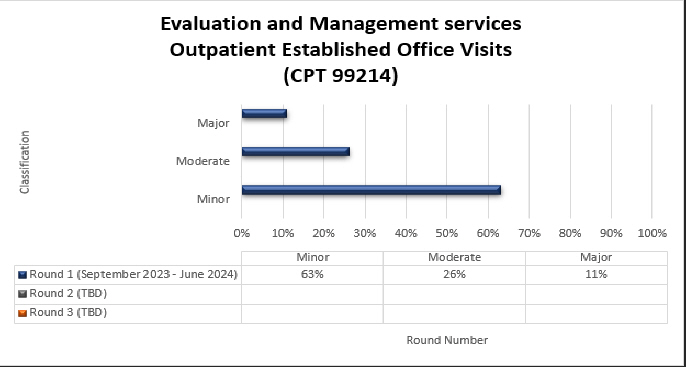
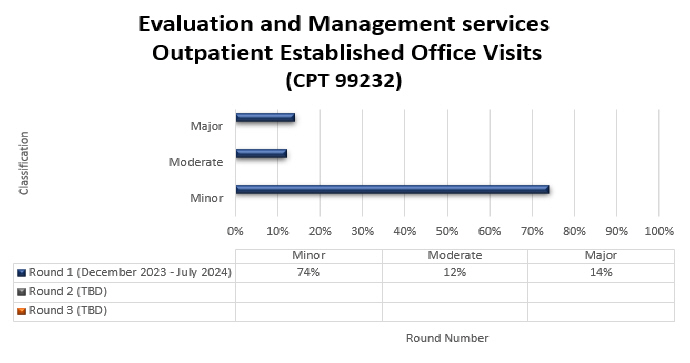
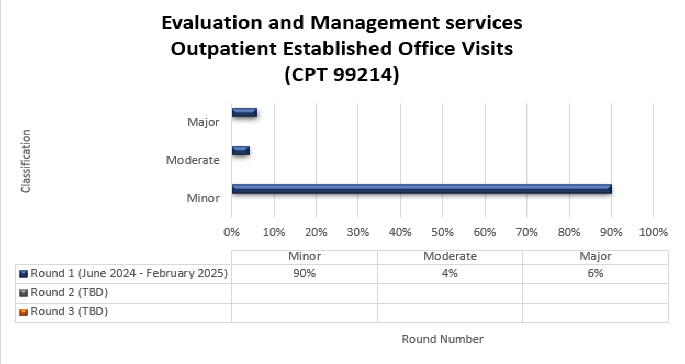
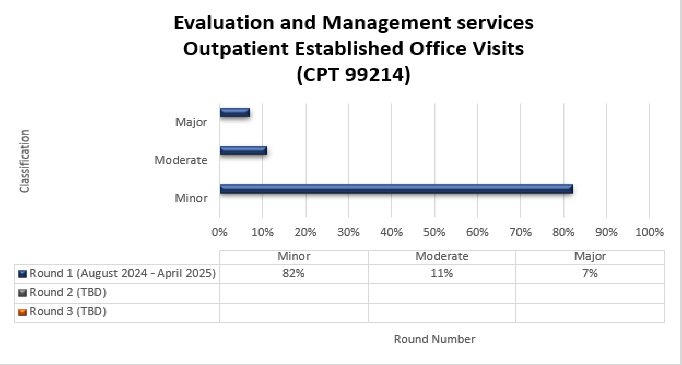
Top denial/partial denial reasons and high-level results are listed below from each round of Evaluation and Management (E/M) services TPE reviews that have been conducted thus far by Medical Review. If you have questions about your individual results, please contact the nurse reviewer assigned to your review for additional information. Additional rounds of review will be utilized when the targeted topic demonstrates a continued need for review with newly identified providers.
The most common reasons for denial or partial denials are the following:
1.
Medical Necessity – The documentation submitted does not support medical necessity as listed in coverage requirements.
2. Insufficient Documentation – Insufficient documentation was provided to support the services as billed to Medicare. Medical Review makes multiple attempts to correct these error types before completion of the review. Below are the following denial reasons for insufficient documentation that we were not able to resolve:
• Documentation submitted for review did not support the level of care billed.
• Documentation submitted for review did not support the billing of the service as “incident to” a physician.
• Documentation submitted did not support the billed services.
• Documentation lacked a comprehensive assessment.
• Documentation submitted for review did not support the billed date of service.
• Documentation submitted supported the key elements for a lower level of service.
• Documentation submitted did not support the incident-to criteria was met.
• Documentation submitted was reduced due to a change in rendering provider.
• Documentation did not include a valid signature and/or credentials.
• Documentation did not support the modifier billed to sup[ort a separately identifiable E/M service.
• Documentation submitted was a duplicate for a service previously submitted by the provider.
• Documentation submitted was not legible.
• Documentation does not support a separate E&M service was performed during a global surgery period.
• Documentation submitted was incomplete and/or insufficient to support the service billed.
• The service billed is not a covered Medicare benefit or is an excluded service.
• Payment is included in another service received on the same date (bundled).
• Non-response to documentation request.
99204
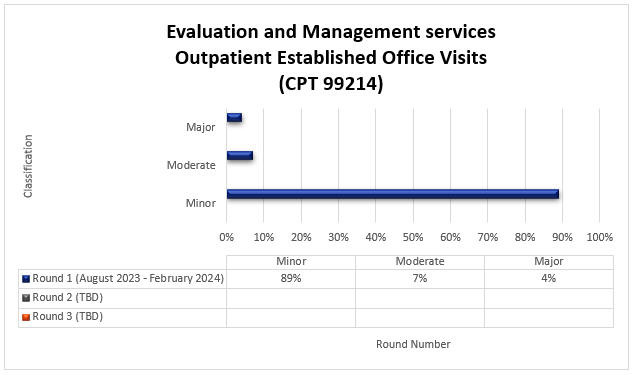
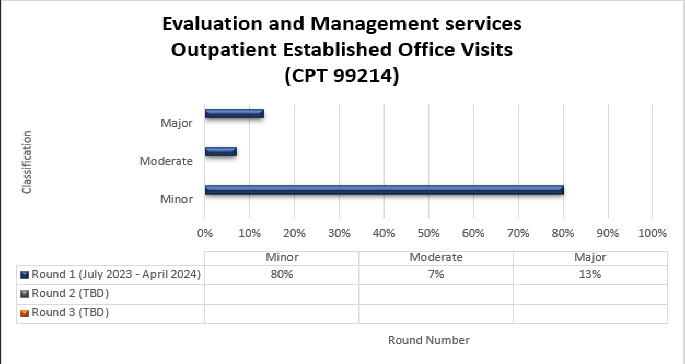
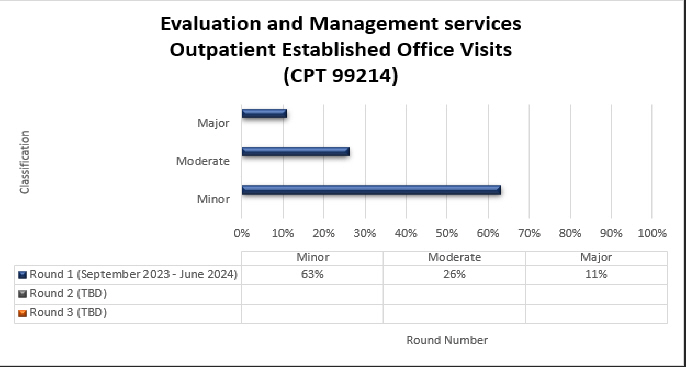
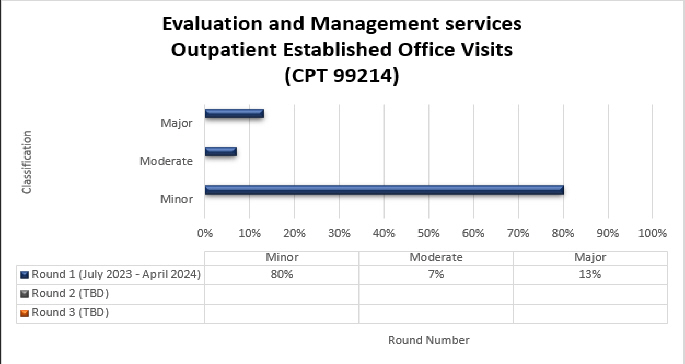
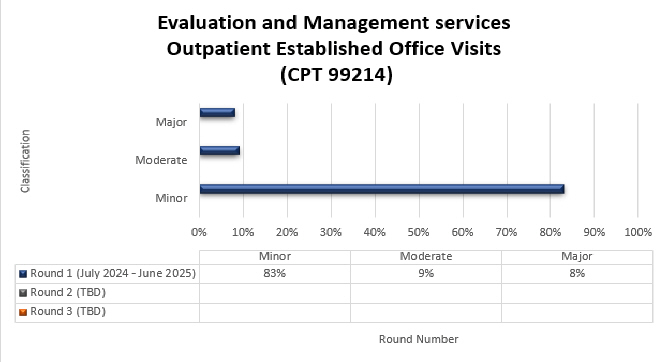
99214
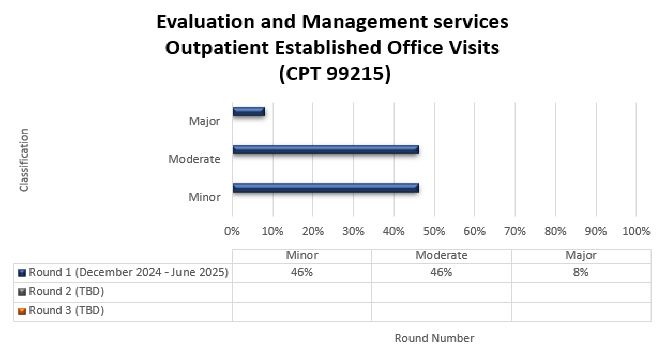
99215
First Coast Service Options (First Coast) strives to ensure that the information available on our provider website is accurate, detailed, and current. Therefore, this is a dynamic site and its content changes daily. It is best to access the site to ensure you have the most current information rather than printing articles or forms that may become obsolete without notice.