COVID-19 vaccine and monoclonal antibody billing for Part A providers
This article will assist Medicare Part A providers with proper billing relating to COVID-19 vaccine and monoclonal antibody (mAb) infusion. Beneficiary coinsurance and deductible are waived.
How to bill for COVID-19 vaccines and monoclonal antibodies
For billing single claims for COVID-19 vaccines and monoclonal antibodies, follow the instructions in the article below:
- For roster billing and centralized billing, reference the Medicare billing for COVID-19 vaccine shot administration page.
For coding, effective dates and payment allowances for COVID-19 vaccines, refer to the CMS vaccine pricing - COVID-19 vaccines and monoclonal antibodies.
The types of bill (TOBs) to report for the COVID-19 vaccine and mAb infusion on the Part A claim form, or electronic equivalent, are:
- Inpatient Part B
- Hospital -- 12X
- SNF -- 22X
- Outpatient
- Hospital -- 13X
- SNF -- 23X
- End stage renal disease -- 72X
- Comprehensive outpatient rehabilitation facility -- 75X
- Critical access hospital -- 85X
- Revenue codes:
- 0771 -- Preventive care services, vaccine administration
- 0636 -- Pharmacy, drugs requiring detailed coding
Note: An attending physician is required on all Part A claims including the COVID-19 vaccine and mAb infusion claims. If there is no attending physician information on the claim, it will be returned with reason code.
For information on dosing intervals, refer to the CDC article Vaccine and Immunizations.
HCPCS M0201(administration of pneumococcal, influenza, hepatitis b, and/or covid-19 vaccine inside a patient's home) is billable only on the following TOBs: 13X, 34X, 72X, 75X, 81X, 82X, and 85X.
For additional billing information on M0201, review the following CMS resources:
- Infographic PDF on Medicare payment for COVID-19 vaccination administration in the home
- Coding for COVID-19 vaccine shots
- Medicare COVID-19 vaccine shot payment
Vaccine billing examples
Billing example for first dose:
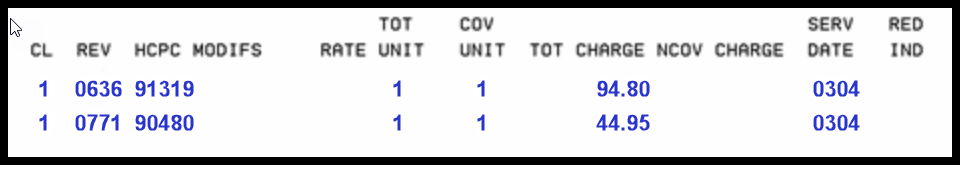

Condition code:
- A6 – 100% payment
Diagnosis code:
- Z23 – Encounter for immunization
- Required as primary diagnosis
Billing example for second dose:
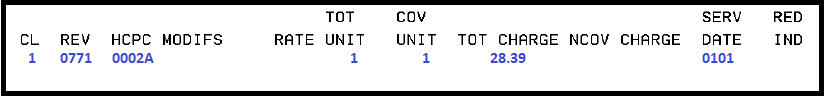
Condition Code:
- A6 - 100% payment

Diagnosis code:
- Z23 - Encounter for immunization

Note: For vaccines provided for inpatients, use the date of discharge or date Part A benefits exhausted as the date of service.
Monoclonal antibodies and their administrations currently authorized
For payment allowances and coding refer to the CMS vaccine pricing - COVID-19 vaccines and monoclonal antibodies and the CMS COVID-19 monoclonal antibodies webpages.
Billing example for infusion:
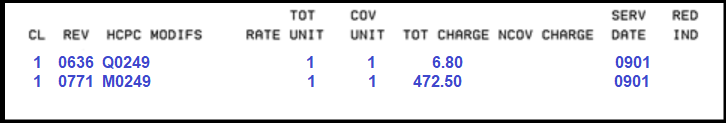

Diagnosis codes:
- Use appropriate diagnosis coded to highest level of specificity
- U071 use as appropriate

Note: For vaccines provided for inpatients, use the date of discharge or date Part A benefits exhausted as the date of service.
Federally qualified health centers (FQHCs) and rural health clinics (RHCs)
Please see CMS IOM Pub. 100-02 Medicare Benefit Policy Manual, Chapter 13, section 220.1, "Preventive Health Services in RHCs" and 220.3, "Preventive Health Services in FQHCs" for current guidelines to bill COVID-19 vaccine administration and monoclonal antibodies.
References
- COVID-19 frequently asked questions (FAQs) on Medicare fee-for-service (FFS) billing
- COVID-19 provider toolkit
- COVID-19 monoclonal antibodies
- Coding for COVID-19 Vaccine Shots
- Medicare billing for COVID-19 vaccine shot administration
- Medicare COVID-19 vaccine shot payment
- Medicare payment for COVID-19 vaccination administration in the home
- Monoclonal antibody COVID-19 infusion