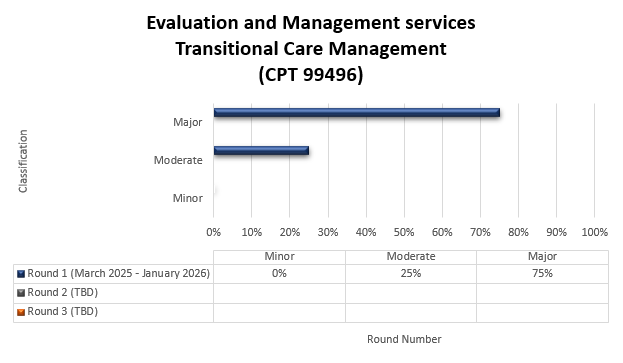
Targeted probe and educate round results: Transitional care management
Top denial/ partial denial reasons and high-level results are listed below from each round of Transitional Care Management (TCM) services TPE reviews that have been conducted thus far by Medical Review. If you have questions about your individual results, please contact the nurse reviewer assigned to your review for additional information. Additional rounds of review will be utilized when the targeted topic demonstrates a continued need for review with newly identified providers.
Top denial/partial denial reasons:
The most common reasons from denial or partial denials are the following:
- Medical Necessity - The documentation does not support medical necessity as listed in coverage requirements.
- Insufficient Documentation - Insufficient documentation was provided to support the services as billed to Medicare. Medical Review makes multiple attempts to correct these error types before completion of the review. Below are the following denial reasons for insufficient documentation that we were not able to resolve:
- Documentation lacked evidence that this date of service is within the required time frame from a discharge date from an inpatient facility.
- Documentation did not support complexity level of medical decision making (MDM) as billed and did not include the patient discharge date.
- Documentation does not support that a form of interactive contact was made or attempted with the beneficiary and/or caregiver within two business days of discharge, which is required element of service billed.
- Documentation submitted did not support incident-to criteria were met.
- Documentation submitted supported the key elements and/or reasonable necessity of a lower level of service.
- Documentation submitted supports the performing and billing providers are different.
- Service billed in error.
- Non-response to documentation request.
Round Results